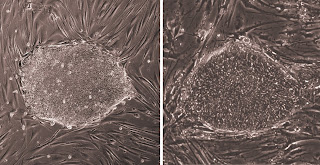
iPS cells and embryonic stem cells — similar but not the same
In the most recent face-off between iPS and embryonic stem cells, the ES cells came out ahead — turns out iPS cells aren’t the same as ES cells even when they carry the same mutation. That’s according to work published in the May 7 issue of Cell Stem Cell.
(The image shows colonies of embryonic and iPS cells, taken taken in the lab of Jeanne Loring at The Scripps Research institute.)
First some background. Embryonic stem cells come from 5-6 day old embryos left over after in vitro fertilization. These primitive cells can turn into all cells of the body. iPS cells come from adult cells — most often the skin — that are reprogrammed to act like embryonic stem cells. They can also form all cells of the body. When iPS cells were first created in 2007 by Shinya Yamanaka, the prevailing wisdom was that they might one day completely replace ES cells, but only if they are safe and are truly equivalent to their embryonic counterparts.
That “but” has been the source of ongoing experiments, many by CIRM-funded researchers, who have found that the two cell types have different genes active (see this blog entry). In this latest work, the European and Israeli researchers found that when they created iPS and ES cells both containing a mutation that causes fragile X syndrome, the two resulting groups of cells behaved very differently, with the iPS cells not even activating the mutated gene.
This finding raises questions about whether iPS cells will be the best choice for mimicking diseases in a dish.
In an article in Medical News Today, Nissim Benvenisty, director of the Stem Cell Unit at the Hebrew University of Jerusalem and a leading author of the study, says:
“Until we understand better the differences between these two types of cells, the optimal approach might be to model human genetic disorders using both systems, whenever possible”.
That said, when Stefan Heller of Stanford University created ear hair cells from both ES and iPS cells he found no difference in their functionality.
A.A.